Bacterial Diversity in Oral Samples of Children in Niger
with Acute Noma, Acute Necrotizing Gingivitis, and
Healthy Controls
Bolivar, I., Whiteson, K., Stadelmann, B., Baratti-Mayer, D., Gizard, Y., Mombelli, A., & ... Rusconi, M. M. (2012).
Description of Noma and Acute Necrotizing Gingivitis
Noma: This disease is alternatively known as Cancrum oris or Gangrenous stomatitis. This disease causes rapid tissue destruction of the face and oral cavity in young children who live in remote, undeveloped countries. African children are most commonly afflicted with this disease due to poor nutrition, unclean living conditions, and unclean drinking water to name a few. This is an opportunistic infection and can lead to mortality and morbidity. The authors hypothesized that there may be a link between the bacteria that causes Acute Necrotizing Ulcerative Gingivitis and that the presence of such bacteria might trigger Noma.
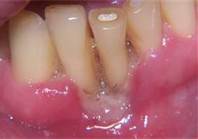
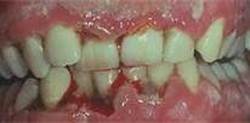
Acute Necrotizing Ulcerative Gingivitis (ANUG/NUG): also known as Trench mouth, or Vincent's infection, Vincent's Stomatitis. This is an acute infection of the gingiva characterized by painful ulcerative gingiva, halitosis and bleeding. This occurs suddenly.
Acute Necrotizing Ulcerative Gingivitis (ANUG/NUG): also known as Trench mouth, or Vincent's infection, Vincent's Stomatitis. This is an acute infection of the gingiva characterized by painful ulcerative gingiva, halitosis and bleeding. This occurs suddenly.
Distinguishing Diagnostic Factors
Noma: Physical examination show inflamed areas of the oral cavity such as ulcers, gingival tissue destruction, facial destruction, bone destruction. Drainage of the infection is also seen and is foul smelling.
NUG: Presents with pain, bleeding, gingival ulceration. There is a presence of a pseudomembrane film that when rubbed off reveals a raw painful area. The pseudomembrane consists of necrotic epithelial cells, plaque and microbial organisms. The interdental papilla is necrotic and appears as punched out. Patients with necrotizing ulcerative gingivitis present with halitosis as well. Some signs and symptoms include fever, bleeding upon gentle touch and regional lymphadenopathy. Unlike, Necrotizing Ulcertative Periodontitits, NUG is limited to the gingival tissues only.
Etiology of Disease or Condition
The specific cause of Noma is unknown but studies have shown that bacterial organisms show to play a factor. It is similar to NUG in which there are similar bacteria such as P. intermedia, Fusobacterium species, Borrelia and Treponema.
Predisposing factors for Noma
Malnutrition, dehydration, poor oral hygiene, poor sanitation, AIDS, unsafe drinking water, presence of NUG
Predisposing factors for NUG:
Impaired host response, nutrition, smoking, stress, fatigue, psychosocial factors, systemic disease, alcohol abuse, or drug abuse, may also be due to immunosuppression seen in HIV infection. A previous study was done showing that this same bacteria was introduced into healthy tissues, yet did not produce a disease. It was then hypothesized that there are other host factors in conjunction with the bacterial organisms, which will manifest the disease
Predisposing factors for Noma
Malnutrition, dehydration, poor oral hygiene, poor sanitation, AIDS, unsafe drinking water, presence of NUG
Predisposing factors for NUG:
Impaired host response, nutrition, smoking, stress, fatigue, psychosocial factors, systemic disease, alcohol abuse, or drug abuse, may also be due to immunosuppression seen in HIV infection. A previous study was done showing that this same bacteria was introduced into healthy tissues, yet did not produce a disease. It was then hypothesized that there are other host factors in conjunction with the bacterial organisms, which will manifest the disease
Pathogens Associated with Disease or Condition
Noma: Borrelia vincentii, Porphyromonas gingivalis, Tannerella forsynthesis, Treponema denticola, Staphylococcus aureus are found in samples.
NUG: Borrelia vincentii, P. intermedia, Fusobacterium species, Borrellia and Treponema.
NUG: Borrelia vincentii, P. intermedia, Fusobacterium species, Borrellia and Treponema.
Classification of the Disease or Condition Using the AAP Classification System
Noma: Plaque induced gingival diseases modified by malnutrition: Type I-A
NUG: Plaque induced gingival disease. Necrotizing gingival disease Type 1-A
NUG: Plaque induced gingival disease. Necrotizing gingival disease Type 1-A
Prevalence of the Disease or Condition
Noma: Most commonly seen in children between 2-9 yrs of age. Sex predilection: Equal between males and female. It is seen mostly between October to April.
NUG: Can occur in patients of all ages. The highest incidences are seen between the ages of 20-30. It is also more common in undeveloped countries.
NUG: Can occur in patients of all ages. The highest incidences are seen between the ages of 20-30. It is also more common in undeveloped countries.
Factors to Include in Patient Education
Good oral hygiene is important. Patients need to be educated on how to decrease the amount of plaque and bacterial count. Oxygenating mouth rinses will help aid in decreasing the amount of bacteria. Patients need to also be educated on how if the situation is left untreated, the disease can progress. NUG may progress to Noma, and that can progress to severe facial and functional deformities.
Treatment Recommendation or Corrective Procedures
Noma: The initial management for Noma is usually ulcer debridement and medication. Improvement in oral hygiene and nutritional status is very important as well. In advance destructive cases, reconstructive surgery is necessary after initial treatment with antibiotics. Many patients that present with Noma require treatment for TMJ, extraction and teeth prosthesis.
NUG: Treatment for NUG patients should be in a series of planned out appointments. It is recommended that in the first appointment, the pseudomembrane should be removed with gentle irrigation and cotton. Supragingival periodontal instrumentation can be done, but must be limited due to discomfort for the patient.
2 days after the initial treatment, subgingival instrumentation can be performed and further OHI.
5 days after initial treatment, completion of subgingival instrumentation is performed.
In advanced cases, a therapeutic dose of antibiotics can be given as an early management type.
Lesions should clear up in about 2-3 weeks and afterwards a comprehensive clinical assessment should be performed to check for any underlying chronic periodontal disease.
Patient instructions for the first visit include proper OHI such as toothbrushing restricted to very soft bristles to remove debris. Daily rinses twice a day with chlorhexidine and hydrogen peroxide with water to oxygenate the area will help as well.
NUG: Treatment for NUG patients should be in a series of planned out appointments. It is recommended that in the first appointment, the pseudomembrane should be removed with gentle irrigation and cotton. Supragingival periodontal instrumentation can be done, but must be limited due to discomfort for the patient.
2 days after the initial treatment, subgingival instrumentation can be performed and further OHI.
5 days after initial treatment, completion of subgingival instrumentation is performed.
In advanced cases, a therapeutic dose of antibiotics can be given as an early management type.
Lesions should clear up in about 2-3 weeks and afterwards a comprehensive clinical assessment should be performed to check for any underlying chronic periodontal disease.
Patient instructions for the first visit include proper OHI such as toothbrushing restricted to very soft bristles to remove debris. Daily rinses twice a day with chlorhexidine and hydrogen peroxide with water to oxygenate the area will help as well.
Maintenance Recommendation:
Proper nutrition and hydration is imperative in maintaining adequate oral health care for Noma and NUG patients. Dietary supplements should be taken in concurrence with good oral hygiene and frequent oral debridement.
References
1. Adeola, D. S., & Obiadazie, A. C. (2009). Protocol for managing acute cancrum oris in children: An experience in five cases. African Journal Of Paediatric Surgery, 6(2), 77-81. doi:10.4103/0189-6725.54767
2. Bolivar, I., Whiteson, K., Stadelmann, B., Baratti-Mayer, D., Gizard, Y., Mombelli, A., & ... Rusconi, M. M. (2012). Bacterial Diversity in Oral Samples of Children in Niger with Acute Noma, Acute Necrotizing Gingivitis, and Healthy Controls. Plos Neglected Tropical Diseases, 6(3), 1-11.
3. Finkelstein, M. W., & Vincent, S. D. (2004). MAXILLOFACIAL PATHOLOGY: Management of Mucosal and Related Dermatologic Disorders. In , Peterson's Principles of Oral & Maxillofacial Surgery (pp. 679-695). People's Medical Publishing House USA Ltd (PMPH).
4. Geneva Study Group on Noma. Retrieved October 20, 2012, from http://www.gesnoma.org/about_noma.php
5. Nield-Gehrig, Jill S., Willmann, Donald E. Foundations of Periodontics for the Dental Hygienist. 3rd Edition 2011.
2. Bolivar, I., Whiteson, K., Stadelmann, B., Baratti-Mayer, D., Gizard, Y., Mombelli, A., & ... Rusconi, M. M. (2012). Bacterial Diversity in Oral Samples of Children in Niger with Acute Noma, Acute Necrotizing Gingivitis, and Healthy Controls. Plos Neglected Tropical Diseases, 6(3), 1-11.
3. Finkelstein, M. W., & Vincent, S. D. (2004). MAXILLOFACIAL PATHOLOGY: Management of Mucosal and Related Dermatologic Disorders. In , Peterson's Principles of Oral & Maxillofacial Surgery (pp. 679-695). People's Medical Publishing House USA Ltd (PMPH).
4. Geneva Study Group on Noma. Retrieved October 20, 2012, from http://www.gesnoma.org/about_noma.php
5. Nield-Gehrig, Jill S., Willmann, Donald E. Foundations of Periodontics for the Dental Hygienist. 3rd Edition 2011.